A study completed by Mount Royal alumni Tyler Faulds in partnership with AIDS Calgary Awareness Association and the Southern Alberta Clinic suggests that levels of depressive and anxious symptoms may influence medication adherence behavior in Albertan men living with HIV.
The study, which was completed as an undergraduate thesis spanning nine months, was an attempt to shed light on two key statistics. First, people living with HIV are far more likely to experience anxiety and depression – some estimates include up to 10x more likely. Secondly, at any given time 30% of people undergoing HAART therapy are not perfectly precise with their medication – a behavior which has potentially dangerous health effects for the individual. The possible connection between these two factors has been studied extensively, most usually assuming that depression leads to poor motivation, or to learned helplessness. That is, someone with HIV just learns to give up over time. Both of these approaches ignore the strength and the diligence of the HIV and AIDS communities, and so Faulds proposed inner speech as a more likely mediating factor.
Inner speech or the voice inside all of our heads that narrates, comments on, and reflects on our day to day interactions plays a more important role than at first glance. Inner speech may actually influence our motivations, feelings, self-concepts, attitudes, and relationships. This voice – that can do everything from remind us to walk the dog, put ourselves down, and focus on our own failures – is a finite resource; only so much can be thought about at any one time. The link proposed by Faulds is that a person living with HIV has more varied and more numerous things to think about than a comparable person without HIV. While someone without HIV may talk to themselves about their goals or their plans for the evening – a person living with HIV might do all of the same things but also think about their health, their partner’s health or their own mortality. They might think about how others see them, an activity magnified by the stigma that HIV+ persons still face. Add on concerns about depression and anxiety – which can include sadness, nervousness, uneasiness and more, and the amount of inner speech available quickly diminishes. Previous studies have shown that the most frequent function of inner speech in the general population is to help plan out future tasks, and to remind people about those tasks and to complete them. Perhaps when someone living with HIV also suffers from depression and anxiety the first place that they lose inner speech capacity is when thinking about future tasks. Without as many cognitive resources to devote to planning out future tasks and reminding us to complete them, a person living with HIV simply does not have the capacity left to remember to take their medication.
Equal groups of HIV+ and HIV- men took part in the study to examine this potential relationship. They completed measures of depressive and anxious symptoms, provided basic demographic information, and also provided ten examples each of their own past inner speech. Participants were asked to recall ten times they had talked to themselves in the recent past and to input them into the online survey. An example response given by a participant was “I thought about past relationships and the reasons that they did not work out”. Each response was coded for its content (what the speech was about) its function (what was the purpose of the speech) and its frequency (how many times a similar inner speech instance was provided). All of these factors were considered for both groups and were then compared.
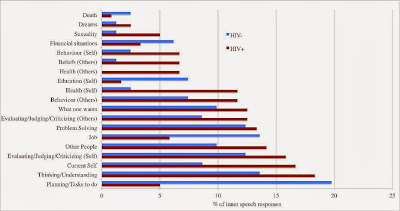
HIV+ men scored higher on measures of depression and anxiety than HIV- men. When their inner speech patterns were compared some key differences became evident. The graphic of these frequency, function and content comparisons is shown below:
While HIV+ men were consistently more likely to think about their sexuality, their own behavior, their health and the health of others – men who do not have HIV were more concerned with their jobs and their educations. The most interesting comparison of all, and the one with the largest disparity between groups was on how often the groups talked to themselves about planning future tasks to complete. While HIV- men considered this inner speech function nearly 20% of the time, HIV+ men only utilized this function 5% of the time. This difference supports the hypothesis– that men living with HIV are far more preoccupied with other concerns, and consequently have less inner speech time to devote to planning out future tasks.
The next link in this chain of investigation would be to repeat the study but directly report the adherence behavior of its participants. If this could then be correlated to the existing comparison – that as levels of depression and anxiety increase the amount of time devoted to planning out future tasks decreases – then the link would be solidified. In the meantime this study offers a few key recommendations and cautions.
For cautions – the results of this study suggest a connection but cannot concretely prove one. If you are someone living with HIV, it does not mean that you are bad at remembering to do things. It also does not mean that you are depressed. One of the most inspiring things about the HIV+ community is how diverse the experiences of its members are. This study looked at general trends only.
For recommendations – especially to service providers, there are two. First, make the psychological health of your clients as important as their physical health. One often overlooked detail is that besides working on ways to keep the body healthy, the mind is an organ which needs to be taken care of as well. Secondly, programs which try to teach proper adherence behavior need to alter their approaches. Rather than hitting a nail on the head with “Remember, remember, remember,” consider that other concerns may be in the way. Once they are dealt with, adherence may come much easier.
For any questions or comments regarding the study, readers are encouraged to contact the researcher directly. Feel free to do so at [email protected]
References:
Canadian HIV Legal Network. (2011). HIV/AIDS policy and law review.
http://www.aidslaw.ca/publications/interfaces/downloadFile.php?ref=2022
Accessed November 2012.
Crepaz, N., Passin, W. F., Herbst, J. H., Rama, S. M., Malow, R. M., Purcell, D. W., &
Wolitski, R. J. (2008). Meta-analysis of cognitive-behavioral interventions on
HIV-positive persons’ mental health and immune functioning. Health Psychology,
27(1), 4–14. doi:10.1037/0278-6133.27.1.4
Du Bois, S. N., & McKirnan, D. J. (2012). A longitudinal analysis of HIV treatment
adherence among men who have sex with men: A cognitive escape perspective.
AIDS care, 24(11), 1425–1431. doi:10.1080/09540121.2011.65067
Gonzalez, J. S., Penedo, Antoni, M. H., Durán, R. E., McPherson-Baker, S., Ironson, G.,
& Schneiderman, N. (2004). Social support, positive states of mind, and HIV
treatment adherence in men and women living with HIV/AIDS. Health
Psychology, 23(4), 413–418. doi:10.1037/0278-6133.23.4.413
Johnson, J. G., Alloy, L. B., Panzarella, C., Metalsky, G. I., Rabkin, J. G., Williams, J. B.
W., & Abramson, L. Y. (2001). Hopelessness as a mediator of the association
between social support and depressive symptoms: Findings of a study of men with
HIV. Journal of Consulting and Clinical Psychology, 69(6), 1056–1060.
doi:10.1037/0022-006X.69.6.1056
Morin, A., Uttl, B., & Hamper, B. (2011). Self-reported frequency, content, and functions
of inner speech. Procedia-Social and Behavioural Journal, 30, 1714-1718
Morin, A. (2005). Possible links between self-awareness and inner speech. Journal of
Consciousness Studies, 12(4), 115–134.
Uttl, B., Morin, A., Faulds, T., Hall, T., & Wilson, J. (2012). Sampling inner speech
using text messaging. Poster presented at the CSBBCS conference (Kingston,
ON) on June 7-9, 2012.